Understanding the difference between allergies vs COVID is especially important this time of year because there’s a lot of overlap in symptoms, which can be stressful for parents.
Allergy season is in full swing—pollen levels are high, kids are spending more time outside, and it’s very common to see symptoms like congestion, coughing, and fatigue start to show up.
Those symptoms can begin to feel confusing. Is it just allergies… or something else?
Why Allergies vs COVID Symptoms in Kids Can Be Confusing
It’s easy to mix these up because many of the symptoms look similar at first.
Both allergies and viral illnesses can cause congestion, coughing, headaches, and fatigue. And in younger children, it’s not always easy to tell how they’re feeling or when symptoms started.
The key isn’t just what symptoms are present—it’s how they show up, how long they last, and what patterns you notice.
Allergies vs COVID: A Side-by-Side Comparison
This is where it can be helpful to step back and look at the bigger picture. This table highlights some of the most helpful differences to look for.
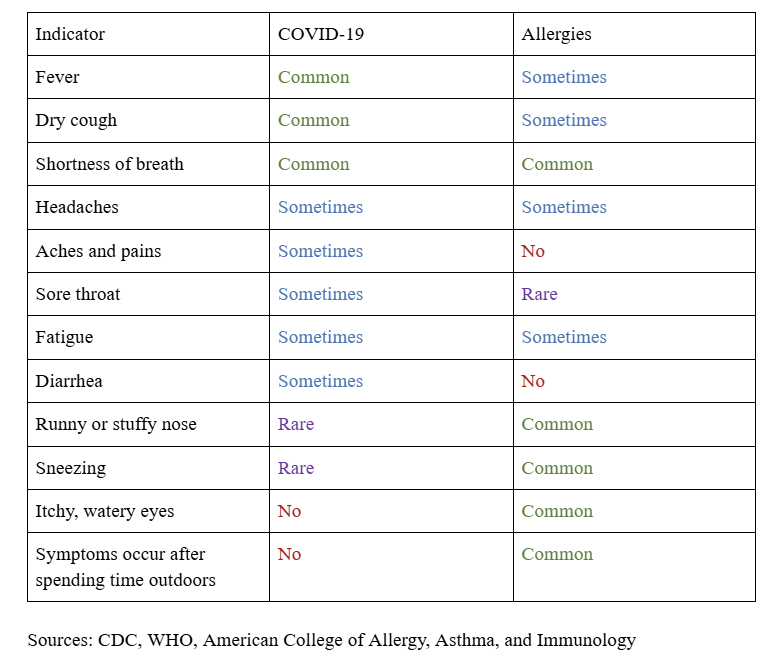
A few key takeaways:
- Fever and body aches are more common with COVID than with allergies
- Itchy eyes and sneezing strongly point toward allergies
- Symptoms after outdoor exposure are a major clue to allergies
- Runny nose and congestion are common in both, which is why confusion happens
Allergies vs COVID: Patterns That Matter
Beyond individual symptoms, patterns over time are often the biggest clue.
Allergies tend to follow a more predictable pattern. Symptoms may come on gradually, last for weeks, and often fluctuate based on exposure, especially time spent outdoors.
Viral illnesses, including COVID, are more likely to come on suddenly and evolve over a few days. You may see a clearer progression, with symptoms either improving or worsening relatively quickly.
Looking at how symptoms behave over time can often give you more clarity than any single symptom.
What’s Happening in the Body During Allergies
When your child is exposed to pollen or environmental triggers, the immune system releases histamine.
Histamine is responsible for classic allergy symptoms, but it also affects the brain.
This is why some children during allergy season may seem more sensitive, reactive, or have more difficulty with focus and sleep.
Histamine acts as an excitatory neurotransmitter, meaning it can increase nervous system activity and make everything feel a bit more intense.
How to Support Your Child During Allergy Season
The goal isn’t just to manage symptoms in the moment, but to support the body so it can respond more appropriately to triggers.
Start with Histamine Support
HKHM Hist-Assist is designed to support the body’s natural ability to regulate histamine and maintain a more balanced immune response.
This can be especially helpful during peak allergy season when exposure is higher and symptoms are more noticeable.

Take a More Comprehensive Approach When Needed
If your child tends to have more persistent symptoms—or a history of asthma, eczema, or recurrent allergies—it can help to take a broader approach.
The HKHM Allergy Bundle combines:
- Histamine support
- Gut support
- Inflammatory balance
This helps address multiple layers of the immune response rather than focusing on just one piece.

When to Take the Next Step
If symptoms are unclear, changing quickly, or not following a typical allergy pattern, it’s always appropriate to check in with your pediatrician.
The goal isn’t to diagnose everything perfectly at home, but to feel more confident in what you’re seeing and how you’re supporting your child.
If you’d like support navigating allergy season—and other recurring childhood illnesses with overlapping symptoms (such as eczema and asthma), please book a free 15-minute informational call with one of our patient care coordinators.
References:
- National Institutes of Health. Is It Flu, COVID-19, Allergies, or a Cold? NIH News in Health. January 2022.
- Hagemann J, Onorato GL, Jutel M, Akdis CA, Agache I, Zuberbier T, Czarlewski W, Mullol J, Bedbrook A, Bachert C, Bennoor KS, Bergmann KC, Braido F, Camargos P, Caraballo L, Cardona V, Casale T, Cecchi L, Chivato T, Chu DK, Cingi C, Correia-de-Sousa J, Del Giacco S, Dokic D, Dykewicz M, Ebisawa M, El-Gamal Y, Emuzyte R, Fauquert JL, Fiocchi A, Fokkens WJ, Fonseca JA, Gemicioglu B, Gomez RM, Gotua M, Haahtela T, Hamelmann E, Iinuma T, Ivancevich JC, Jassem E, Kalayci O, Kardas P, Khaitov M, Kuna P, Kvedariene V, Larenas-Linnemann DE, Lipworth B, Makris M, Maspero JF, Miculinic N, Mihaltan F, Mohammad Y, Montefort S, Morais-Almeida M, Mösges R, Naclerio R, Neffen H, Niedoszytko M, O’Hehir RE, Ohta K, Okamoto Y, Okubo K, Panzner P, Papadopoulos NG, Passalacqua G, Patella V, Pereira A, Pfaar O, Plavec D, Popov TA, Prokopakis EP, Puggioni F, Raciborski F, Reijula J, Regateiro FS, Reitsma S, Romano A, Rosario N, Rottem M, Ryan D, Samolinski B, Sastre J, Solé D, Sova M, Stellato C, Suppli-Ulrik C, Tsiligianni I, Valero A, Valiulis A, Valovirta E, Vasankari T, Ventura MT, Wallace D, Wang Y, Williams S, Yorgancioglu A, Yusuf OM, Zernotti M, Bousquet J, Klimek L. Differentiation of COVID-19 signs and symptoms from allergic rhinitis and common cold: An ARIA-EAACI-GA2 LEN consensus. Allergy. 2021 Aug;76(8):2354-2366. doi: 10.1111/all.14815. Epub 2021 May 14. PMID: 33730365; PMCID: PMC8250633.







