When nine-year-old Javier and his mother first came to see me in 2006, he was having terrible stomach pains and was missing a lot of school. He was a patient of one of the other doctors in the office, but since his schedule was full, Javier was put on my schedule for this same-day sick visit.
His chart was about two inches thick (yes, I practiced when we still used paper charts), and while my schedule didn’t permit me to read the whole thing before his visit, I spent two hours over the next two evenings going through his records.
Recurrent Illnesses with No Relief
It was eye opening. Javier had been on seven rounds of antibiotics in just two and a half years. Four of those were for strep throat, one for pneumonia, and two were for sinusitis. He had also been to the clinic twice for viral gastroenteritis (diarrhea). He was now having these terrible stomach aches and was constipated on top of all of these recurrent illnesses.
I didn’t understand why one child would be getting sick so often. The only thing I knew to do at that time was to start him on the prescription laxative called Miralax® (polyethylene glycol 3350). I knew this was just a BAND-AID® for the situation. My question became: how do I figure out what is causing not only the constipation, but also his recurrent illnesses?

Luckily, I had just learned about a blood test that would allow me to check my patients for food and environmental allergies right in the office. It was a simple blood test I could use in certain situations instead of having to refer patients to an allergist for skin-prick testing all the time. I devoured the information I had at hand, then I called the medical director of the company to clarify what I didn’t understand and dipped my toes into the world of allergies and nutrition with Javier.
Does Your Child Need Allergy Testing?
General pediatrics is filled with kids who have chronic runny noses, poorly controlled eczema and asthma, and many of them need allergy testing. I was referring one or two patients a week to the allergist. The kids would go and get their allergy testing done and the allergist would put them on three or four meds to control their symptoms, an antihistamine, a nasal steroid spray, topical steroids for the eczema, and a stronger inhaled steroid for the asthma. Families would come back to me and not be happy with having to take so many meds.
I ordered the food and environmental allergy panels on Javier. The technical term for this blood work is a serum IgE panel. It looks at the same protein that skin prick tests do, the test you get when you go see an allergist and they prick your back with a variety of allergens. The thought of saving patients a trip to the allergist, a $30 to $70 copay, and giving me better continuity with the child regarding his allergy treatment was very appealing.
Of course, I will always need to refer to allergists; I do not even begin to pretend I understand allergies to the depth and breadth of a trained allergist. I simply see myself as the first line of defense for my patients and their families.
Food and Environmental Allergy Testing
Many things came up positive for allergies on Javier’s allergy test results. Most of the foods we tested were positive, as were the environmental allergens. These results both surprised and didn’t surprise me. The surprising part was that he did not have what we think of as classic environmental allergy type symptoms, runny nose, watery itchy eyes, and a cough. Instead, he had constipation, abdominal pain, and recurrent strep throat.
Food Allergy Testing Results
What started to make sense is that what he was eating and being exposed to in his environment, were triggering the inflammation that was contributing to a lot of his symptoms. The foods that tested positive for Javier were, egg white, milk, codfish, soybean, corn, and peanuts.

Allergy testing may find these common food allergies and sensitivite
Environmental Allergy Testing Results
The environmental allergy testing results were all categorized as indoor allergens: cat, dog, cockroaches, dust mites (two different species), and mold (four different species that can be found indoors and outdoors).
Mattresses and pillows are dust mite havens. One study, conducted at a London hospital, found that after two years, up to a third of a pillow’s weight could be made up of bugs, dead skin, and dust mites and their feces.1
This is when the idea of an overflowing cup of inflammation came to me. Here’s Javier’s, before and after he started the Healthy Kids, Happy Moms program.
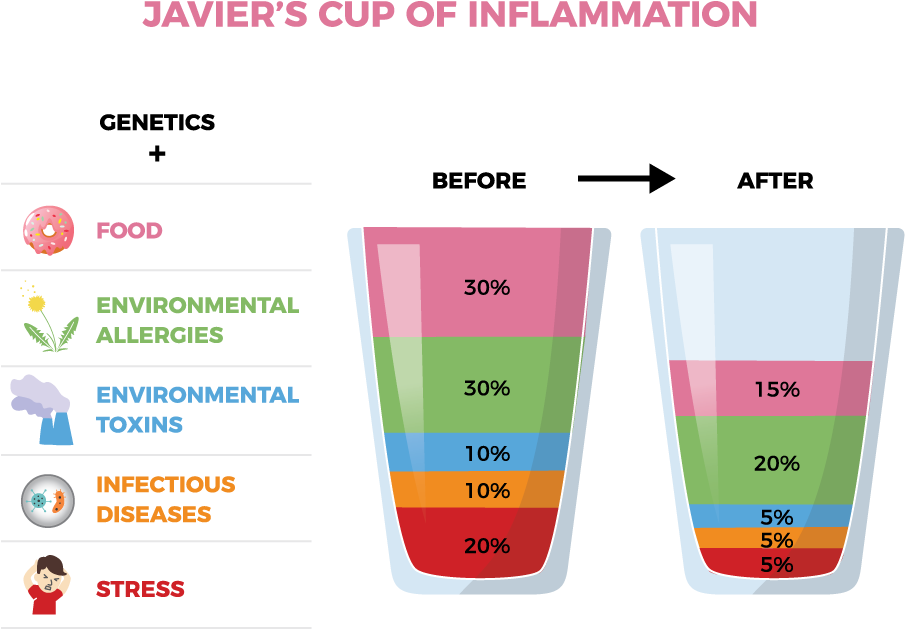
I prescribed an EpiPen® for Javier’s peanut allergy and referred him to a pediatric allergist to help us navigate all of these allergies. In the meantime, I asked his mother to take him off all the foods he tested positive for. I had no idea at the time how difficult it would be for the family to radically change Javier’s diet. But Javier’s symptoms were so severe and chronic that his mother was willing to try it.
Within a week, Javier’s symptoms began to improve. I couldn’t believe what I was seeing but I also knew it was not a coincidence. His symptoms were directly related to the food he was eating. His abdominal pain resolved very quickly, and his bowel movements became easier and easier. Eventually he was having an easy daily bowel movement and we were able to wean him off the Miralax®.
Working with School Cafeterias
I remember his case so well, not only because it was the first time, I had to fill out a school dietary form, but also because he began to improve so quickly off of those foods. All of a sudden, a family I was seeing almost monthly, was not coming in as much.
I was able to stay in touch with his case because of that school dietary form. His mother had to be vigilant with the school so they would honor the changes in his diet that we were implementing, so I had to get very precise on the form, giving the cafeteria examples of what foods might contain dairy, for example. When she saw what profound improvements he had in his health, she was highly motivated to maintain the right nutrition for him at home and at school.
A month later when Javier came in for a check-in visit. I couldn’t believe the change in him. Some foods that are marketed as healthy were actually making him sick, and removing them from his diet could restore his health. He continued to do great and didn’t need a single round of antibiotics that following year.
Processed Foods, Sugar, and the Immune System
Javier’s case helped me correctly deduce two things. First, once his systemic inflammation was in the right balance, his immune system could function more efficiently. Second, by decreasing the processed food he had been eating, the oppressive hold sugar had on his immune system would be lifted and he would be able to move out of the sick cycle.2
A gut that is inflamed or “leaky” cannot absorb nutrients effectively and efficiently from food, let alone from supplements. We start supplements slowly so they can begin to address the irritated gut lining, as illustrated here.
If you would like to see the results that we see in our practice with your kids and other family members at home, you might begin with my online course and book. I have outlined below how to get started.
Shifting the Microbiome with Supplements
My Healthy Kids Happy Moms process is strategically designed first to begin shifting the terrain of your child’s gut microbiome, supporting digestion and absorption of the food. In time, we begin to add in the rest of the foundational supplements, most of which are vitamins, minerals, and fats. I don’t consider them “supplemental,” I consider them necessary nutritional supports to give back what the patient has been depleted of over many years.
The first two supplements we start are a probiotic and a digestive enzyme, which are part of my HKHM foundational bundle.
- Healthy Kids Happy Moms Digest (capsules) OR Healthy Kids Happy Moms Kidz Digest (Berry Flavor Chewable)


Here is a link to our comprehensive integrative supplement guide. It contains all the information you need, including dosing, to get your family started toward better health!
References:
- foxnews.com/health/study-finds-pillows-breeding-ground-for-superbugs(opens in a new tab)foxnews.com/health/study-finds-pillows-breeding-ground-for-superbugs
- Albert Sanchez, J.L. Reeser, H.S. Lau, P.Y. Yahiku, R.E. Willard, P.J. McMillan, S.Y. Cho, A.R. Magie, U.D. Register, Role of sugars in human neutrophilic phagocytosis,The American Journal of Clinical Nutrition, Volume 26, Issue 11, 1973, Pages 1180-1184, ISSN 0002-9165 https://doi.org/10.1093/ajcn/26.11.1180.







